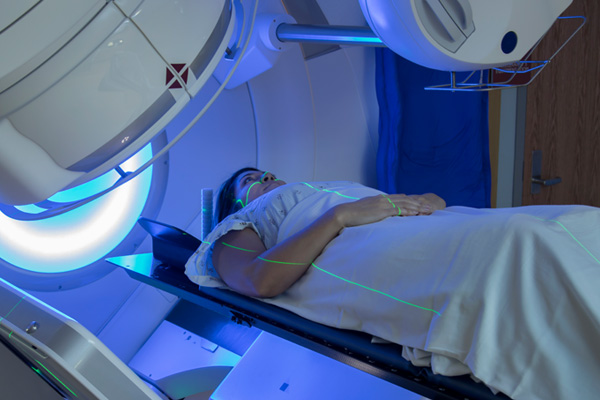
What Are the Treatment Options After a Colon Cancer Diagnosis?
March 02, 2023
This article was reviewed by our Baystate Health team to ensure medical accuracy.
 Daniel R. Fish, MD
Daniel R. Fish, MD

Health & Wellness Tips
Related Articles
Back to Top