Transition to Clinical Training
The 26 members of the Population-based Urban and Rural Community Health (PURCH) Class of 2024 are entering their third year of medical school, and transitioning from classroom learning to clinical training.
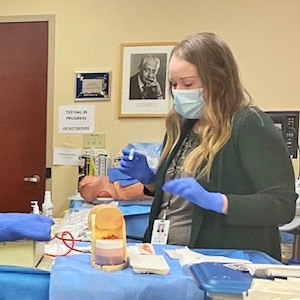
They have spent the last couple of weeks at Baystate's Simulation Center immersed in the Transition to Core Clinical Experiences curriculum. The curriculum includes technical skill training and patient care simulation—designed to prepare them for the greater responsibility they will take on as they become active members of healthcare teams in the hospital, community clinic, or physician's office. (Photo: Amanda Duda, Goldberg Skills Lab Specialist, teaching the students Arterial Blood Gas testing)
Honing Cognitive and Motor Skills
To promote a successful transition to clinical rotations, the curriculum provides hands-on training and introductory skills for their seven required core clerkships: internal medicine, neurology, family medicine, pediatrics, psychiatry, obstetrics/gynecology, and surgery.
Their technical skills training included teaching sessions in airway management, IV access, ABG acquisition, urinary catheter insertion, nasogastric tube insertion, key clinical unit wayfinding, and a review of codes and processes related to emergency situations in various settings.
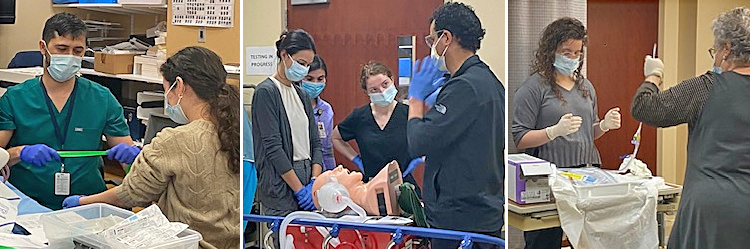
(Photos L to R: IV insertion is taught by Dr. Neil Devoe; Anesthesia resident Dr. Asadullah Siddiqui teaches airway management and bag-valve-mask ventilation; Dr. Halina Wiczyk is teaching urinary catheter insertion)
Like Real Life—But Without the Risk
These third-year students also participated in an exercise that simulated caring for a patient with shortness of breath.
As the full size high-fidelity mannequin lay in the hospital bed, students spoke to him, asked questions and listened carefully. They monitored his pulse, lung sounds, EKG, blood pressure, oxygen levels, and body temperature.
This controlled environment allowed them to safely apply their knowledge, skills, and abilities in diagnosis and case management.
Fourth-Year Students Prepare for More Autonomy
Meanwhile, PURCH's fourth-year medical students were participating in a transition of their own—a week-long simulation skills training readying them for a required acting sub-internship in their field of choice, either medicine, family medicine, surgery, or pediatrics.
Sub-Is are a clinical inpatient opportunity affording students a higher level of autonomy to prepare themselves for internship in a residency program.
"The rising fourth years came to the Sim Center for their Transition to Advanced Studies curriculum, which included ICU based education," said Amanda Duda, Goldberg Skills Lab Specialist. "There was a patient simulation case on acute respiratory failure, as well as technical skills training including ABGs, and IV and Nasogastric tube insertion."